How to manage acute wounds
In this section, you’ll learn:
- how to assess acute wounds
- how to manage acute wounds
- how to create an optimal healing environment
How do I assess acute wounds?
When you assess an acute wound, you should have two main goals. The first is to identify all your patient’s injuries. Remember, that there might be injuries that you can’t see. Your second goal is to identify any potential complications. For example, you want to consider whether the injury is likely to get infected or become non-healing.1
Assessing traumatic wounds
If your patient has an acute traumatic wound, always take a full history of the trauma that caused the wound.1 As you assess the traumatic wound, try to answer the following questions:1
- When did the injury occur?
- How did it happen?
- What type of wound is it?
- How much force was involved in causing the injury?
- Where is it located on the body?
- What are the wound’s characteristics? (size, shape, orientation, wound edges, etc.)
- Is there any soft tissue damage?
- Is there any evidence of a penetrating trauma?
- Is there a foreign body present in the wound?
- Is there a potential underlying structural injury?
Be sure to examine the vascular and neurological status around the injury as well.1
Fact box: When to refer your patient to an emergency department
If you notice any of the following, you should refer your patient to an accident and emergency department:1
- Vascular damage, such as arterial bleeding or loss of pulse;
- Signs of nerve damage, such as loss of sensation or tingling;
- Facial wounds, particularly lacerations that cross the lips, nose or ears;
- Signs of infection in an injury on the palm of the hand;
- A foreign body that’s still in the wound after cleaning; or
- Complex wounds, such as those with irregular edges, wide gaps or damage to underlying structures (e.g. bone).
Assessing surgical wounds
When you assess a surgical wound, you want to identify any risk factors that could lead to delayed healing. You can do this by taking your patient’s complete medical history at the time they’re admitted to your care. It’s particularly important to complete a full medical history before giving the patient anaesthesia.1
As you take the medical history, look for the following risk factors:1
- Your patient’s overall health, immune status and pre-existing medical conditions, e.g. diabetes, cancer or arteriosclerosis;
- Whether the patient has had surgery in the same area before;
- Whether the patient is undergoing other therapies, e.g. radiation therapy, chemotherapy or anticoagulants;
- How long the surgery will last;
- How much blood loss you expect during the surgery;
- Whether wound drains will be placed through the incision; and
- Wound infection.
You should continue to examine the surgical wound during the surgery. Pay particular attention to the soft tissue (e.g. excess scar tissue), and note any damage to nerves, tendons and organs. This way, if complications arise after the surgery, you will know whether the damage happened before or during the surgery.1
How to manage acute wounds
There are five main steps to follow when you manage an acute wound:1
| Step 1: Haemostasis |
|---|
|
Your first step should be to stop the bleeding. To do this, first identify where the bleeding is coming from. You may need to apply pressure, use elevation or use a tourniquet, clamp or suture to stop the bleeding. Stopping the bleeding will also help you to accurately assess the wound. |
| Step 2: Cleanse the wound |
|---|
|
If your patient has a minor acute wound, you can use detergent and water to cleanse it. However, if your patient has a deeper or more complex traumatic wound, you should flush it with a neutral cleansing solution. This will remove any contaminated material. |
| Step 3: Debride the wound |
|---|
|
Most traumatic wounds will be ‘clean’ after you have irrigated them. However, if the wound is devitalised or contaminated you will need to debride it. When you debride the wound, you remove unhealthy or dead tissue from the wound bed. This helps the wound to heal. |
| Step 4: Close the wound |
|---|
|
When you close the wound, you have three main objectives. One, you want to support the tissues until the healing process can restore tensile strength. Two, you want to minimise the risk of bleeding and infection. And three, you want to close the dead space by bringing together the wound edges. This will ensure the best functional and aesthetic result. |
| Step 5: Give medication |
|---|
|
If your assessment reveals that the wound has a high risk of infection, you may choose to prescribe prophylaxis antibiotics. Depending on the type of wound, an analgesic or a tetanus injection might also be necessary. |
How to create an optimal healing environment
Studies show that one of the best ways to help acute wounds heal, is to create a moist wound environment. Creating a moist wound healing environment can help non-healing wounds heal. It can also be effective in managing surgical wound dehiscence.2
Choosing the right dressing
Another important factor in creating an optimal healing environment is the wound dressing. When choosing a dressing for an acute wound, you should consider:
- the wound’s size, shape and location;
- the level of exudate;
- the risk of infection; and
- the conditions of the periwound (surrounding) skin.1
You want to find a dressing that both maintains a moist wound environment and absorbs excess exudate. You can also use dressings to debride the wound (through autolytic debridement) and to treat an infected wound (by using a topical antibacterial dressing).
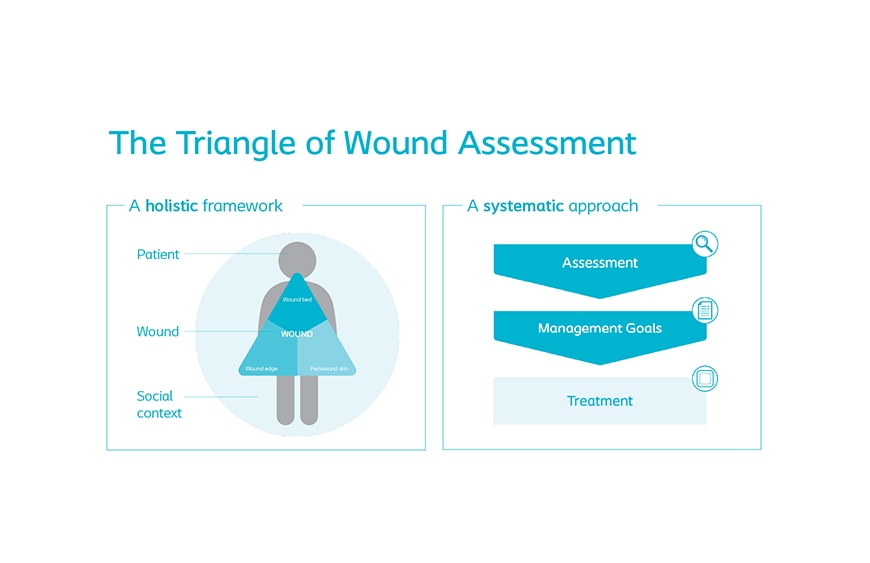
How to conduct a holistic wound assessment
To help you conduct a holistic assessment of the patient and their wound, try using The Triangle of Wound Assessment. This tool will ensure that you are consistent when evaluating the acute wound, and help you to choose the optimal treatment for your patient.
