Get full access with a free account
Benefits of the Coloplast® Professional Educational platform
![]() Full access to educational content, events and resources
Full access to educational content, events and resources
![]() Track your progress
Track your progress
![]() Share content with your colleagues
Share content with your colleagues
![]() Share supporting material with your patient
Share supporting material with your patient

Low Anterior Resection Syndrome
Disordered bowel function (fecal incontinence and/or constipation) can occur after surgical resection of the rectum and impact quality of life.
In 2018, there were 1.8 million cases of colorectal cancer worldwide.1 Advances in surgery and radiation therapy for patients with colorectal cancer have led to improved survival and awareness of post-surgical outcomes.2 Low Anterior Resection Syndrome (LARS) is defined as disordered bowel function after surgical resection of the rectum, often leading to a detriment in quality of life.3 Symptoms range from faecal incontinence and urgency, to constipation and emptying difficulties.2,3
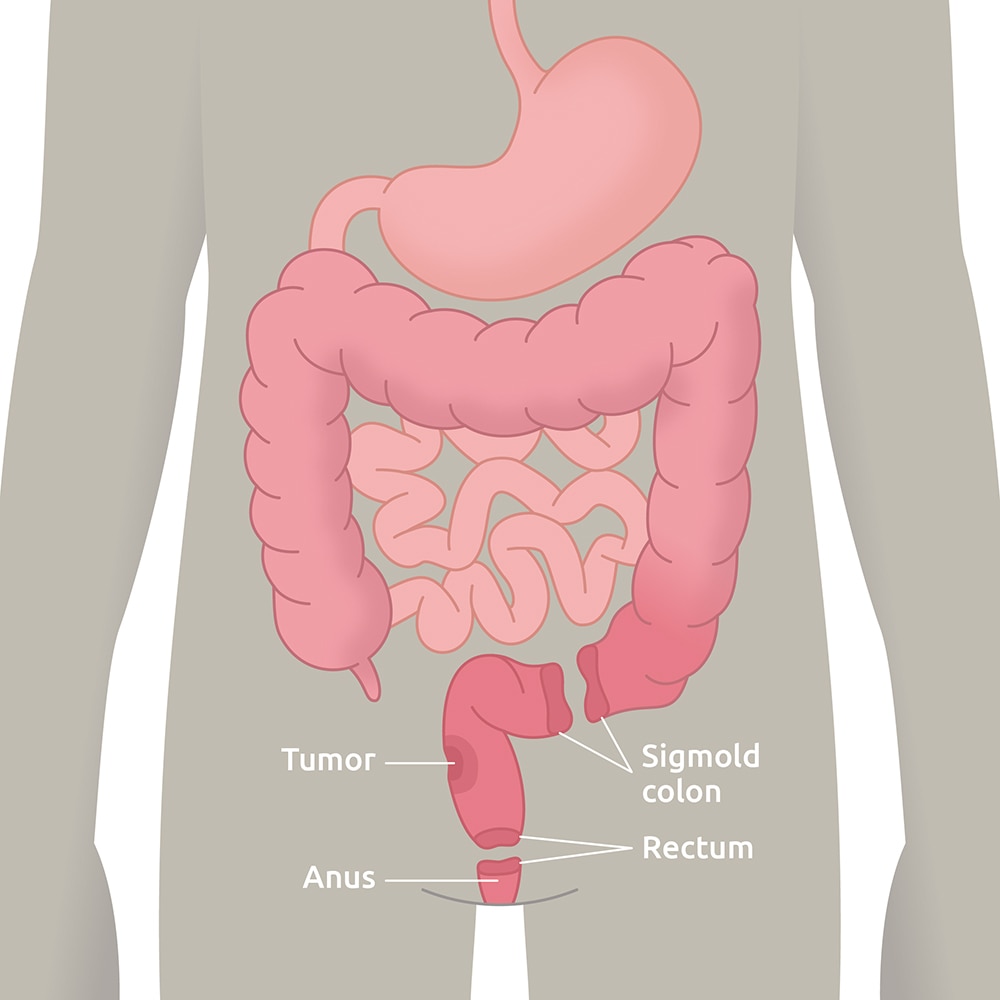
Aetiology
When a diseased or affected portion of the intestine is removed, the remaining sections of the intestine are surgically connected back together.
This surgical connection is called an anastomosis, and there are several types:
- Colon-rectal
- Colon-anus
- J-pouch
As a result, the rectal reservoir decreases in size and increases the likelihood of stool incontinence.4
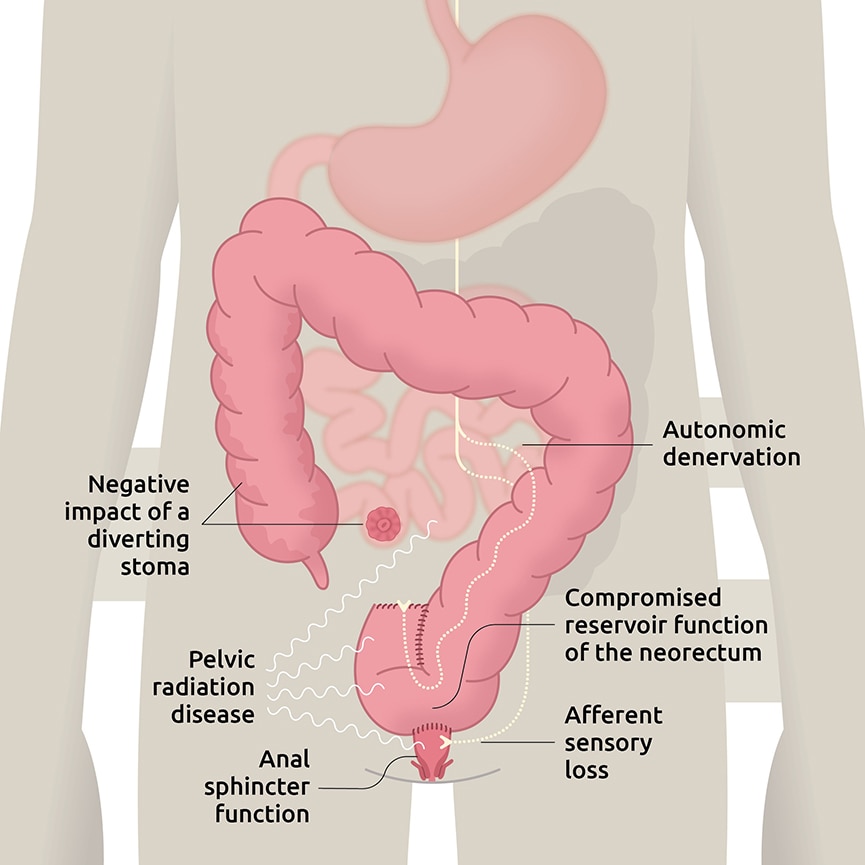
Pathophysiology
Surgical resection of the rectum and the compromised physiologic properties of the neorectum are thought to be the primary cause of LARS, due to change of reservoir function and impaired evacuation.5,6 The length of the rectal remnant correlates with better functional outcomes, but this beneficial effect is lost in patients who received prior neoadjuvant therapy.7 Afferent sensory loss leads to diminished gas-stool discrimination and may cause frequent toilet visits.8 A temporary stoma that is used to avoid anastomotic leak after surgery may also increase the risk of LARS, although the data is conflicting.9-11 Denervation of parasympathetic and sympathetic input increases motility in the proximal colon and interrupts feedback signals in the distal colon that regulate transit.12
In 2021, the LARS Expert Advisory Panel published MANagement gUidelinEs for Low Anterior Resection Syndrome. Read the publication here
Transanal Irrigation (TAI) and LARS
Download the one pager on Clinical Evidence of Peristeen in LARS below.
References
- World Health Organization, 2019. Cancer: Key Facts, 2019. https://www.who.int/en/news-room/fact-sheets/detail/cancer (accessed March 2020).
- Keane C., et al. 2020. International Consensus Definition of Low Anterior Resection Syndrome. Colorectal Dis. 2020 Mar;22(3):331-341.
- Bryant, et al. 2012. Anterior resection syndrome. Lancet Oncol. 2012;13:e403-408.
- Buzatti KCLR & Petroianu A. Pathophysiological aspects of the low anterior resection syndrome for treatment of rectal cancer. Rev Col Bras Cir. 2017;44(4):397-402.
- Machado M, et al. Functional and physiologic assessment of the colonic reservoir or side-to-end anastomosis after low anterior resection for rectal cancer: a two-year follow-up. Dis Colon Rectum. 2005;48(1):29-36.
- Parc Y, et al. Better Function With a Colonic J-Pouch or a Side-to-end Anastomosis?: A Randomized Controlled Trial to Compare the Complications, Functional Outcome, and Quality of Life in Patients With Low Rectal Cancer After a J-Pouch or a Side-to-end Anastomosis. Ann Surg. 2019 May;269(5):815-826.
- Bondeven P, et al. Neoadjuvant therapy abolishes the functional benefits of a larger rectal remnant, as measured by magnetic resonance imaging after restorative rectal cancer surgery. Eur J Surg Oncol. 2015;41(11):1493-9.
- Haas S, et al. Cortical processing to anorectal stimuli after rectal resection with and without radiotherapy. Tech Coloproctol. 2020;24(7):721-730.
- Floodeen H, et al. Evaluation of long-term anorectal function after low anterior resection: a 5-year follow-up of a randomized multicenter trial. Dis Colon Rectum. 2014;57(10):1162-8.
- Gadan S, et al. Does a Defunctioning Stoma Impair Anorectal Function After Low Anterior Resection of the Rectum for Cancer? A 12-Year Follow-up of a Randomized Multicenter Trial. Dis Colon Rectum. 2017;60(8):800-806.
- Keane C, et al. Functional outcomes from a randomized trial of early closure of temporary ileostomy after rectal excision for cancer. Br J Surg. 2019;106(5):645-652.
- Sakr A, et al. Assessment and management of low anterior resection syndrome after sphincter preserving surgery for rectal cancer. Chin Med J. 2020;133(15):1824-1833.
